Reviewed July 2022 to maintain the latest information in treatment and research.
An interview with Thomas Imahiyerobo, MD, Director of Cleft and Craniofacial Surgery.
What is covered under the term craniofacial surgery?
The term craniofacial surgery really refers to surgical procedures that are done within the craniofacial skeleton. Broadly speaking, this is really anything that involves the neck or upward of that area. When we think of craniofacial surgery as a specialty, it really encompasses not only the skeletal aspects of the craniofacial skeleton, so that's bone, cartilage reconstructive work, but also involves procedures and operations that are aimed at treating conditions affecting the soft tissue of the craniofacial skeleton. This includes skin malignancies, congenital birthmarks, as well as any soft tissue or bony trauma.
As a craniofacial surgeon, I find that there are two ways that we think of this field. Number one, we think of it as an anatomic specialty, so again, highlighting areas that need reconstructive or cosmetic work in the clavicle, which is the neck area, and above. But we also think of craniofacial surgery in terms of a set of skills and techniques that we have. Craniofacial specialists are really adept at doing procedures that involve bony work, doing procedures that involve structural changes to the facial skeleton. Moving around bone, skin, or soft tissue from where it is that you have it to where it is that you need it.
What are the most common procedures that you do?
The most common procedures that I'll do as a craniofacial surgeon involve reconstructive work for congenital anomalies that affect the craniofacial skeleton. Things like cleft lip, cleft palate surgery, as well as entities affecting growth of the cranium [skull] itself, such as craniosynostosis. But this also includes more soft tissue work in the craniofacial skeleton, so treatment of congenital birthmarks or hemangiomas, and cartilaginous structures such as treatment of ear malformations or something like microtia, which is a congenital absence of the ear.
What's new in surgical care? Have there been advancements in how you're doing these reconstructions?
There's certainly been a number of exciting and new advancements in the field over the last five to 10 years. One that we have been active participants in here at Columbia includes the use of minimally invasive techniques to treat craniofacial diagnoses.
When I start talking about reconstructive surgery of the facial skeleton, sometimes my patients' eyes open really wide because that sounds maximally invasive. And yet, we've really embraced the use of minimally invasive techniques in order to get the results that we used to do through more maximally invasive approaches. One specific example has been using minimally invasive approaches to treat craniosynostosis, the premature fusion of the cranial sutures, or the cranial growth plates in the skull of a child or an infant. We know that left untreated, in some instances, it can lead to increases in intracranial pressure or issues with future neurocognitive development. It's something that we take very seriously here at Columbia.
How do you treat craniosynostosis minimally invasively?
You know, treating craniosynostosis has always been a large part of my practice. There are many traditional standard techniques that involve open approaches to the craniofacial skeleton, and again, I would put them in the more maximally invasive category. What we've done at Columbia is embrace techniques that can be done through smaller open incisions where we do some limited work at the time of surgery and then are able to use our small access incisions to continue to change the craniofacial skeleton after surgery. These are techniques like distraction osteogenesis, where you can make an osteotomy [cut] in a bone that is not growing well, and connect to the osteotomy a distractor, which you can think of as a device that will lengthen the bone.
Wow. So instead of one big procedure, you’re making changes slowly over time?
Exactly. You put the distractor on and do a smaller procedure, and then subsequently, you can use a distractor to slowly lengthen the bone or move the bone over time. Then the distractors can be removed in another small, outpatient procedure. We can really make big changes in the craniofacial skeleton with this combination of smaller procedural approaches.
That’s pretty amazing.
It is! Another minimally invasive or minimal access technique that we've embraced is the use of endoscopic craniofacial surgery. An endoscope is a small device that has a light and a camera connected to it; you could think of it as a really small fiber-optic camera. So we can make small incisions somewhere in the scalp or the craniofacial area, and then use the endoscope for visualization. And using smaller instruments, we go in and release points of bony fusion, remove bony tumors, and treat entities such as single-suture craniosynostosis.
After you have used the endoscope through the small access incisions, you can then, again, post-operatively, do things to continue to mold the shape of the craniofacial skeleton and overall get a treatment plan that allows you to get to the same endpoint that we used to do with much larger access procedures.
How do non-surgical management options factor into treatment for the conditions you see?
That’s a great question. There are certainly many entities in craniofacial surgery that can be adequately treated non-surgically. What's been exciting in the last five to 10 years is there are some entities that we used to treat primarily surgically that have now moved over to non-surgical treatment. One is the treatment of hemangiomas. Hemangiomas are one of the most common vascular anomalies [congenital, pigmented birthmark] that we see in children. They can be big venous anomalies or capillary malformations, or they can be a collection of small arterials and capillaries that have overgrown.
The treatments for hemangiomas used to be primarily surgical. This involved us sometimes doing moderately-sized procedures on very little children and infants. What we're doing now, in partnership with some of our pediatric dermatology colleagues, is to use medical therapy to either slow the growth of the hemangioma or in some cases actually shrink it down to the point where it resolves. So, we’re either making surgery much smaller or obviating the need for surgical intervention altogether.
One of my colleagues, Dr. June Wu, along with Maria Garzon, MD in pediatric dermatology, have established the Vascular Anomalies Clinic at Columbia. This is a monthly clinic where they see patients from all over the tri-state area and some nationally. They come up with a treatment plan that is a combination of medical therapy, and at times, reserve surgical therapy when medical therapy has not been effective.
Awesome.
Another one is the treatment of congenital ear malformations. Congenital ear malformations are actually the most common congenital malformation of the craniofacial skeleton. They come in two flavors—minor ear malformations and major ear malformations. Minor ear malformations are those where all the parts of the normal ear may be present, however, they may be misaligned or folded or projecting in a way that's not ideal. That's opposed to major ear malformations, such as microtia, where either all of or part of an ear did not develop. At Columbia, we’ve embraced non-surgical treatments for minor ear malformations by using techniques like ear molding.
What is ear molding exactly?
Say a child has a minor ear malformation and is referred to us during the neonatal period, so that means the first six weeks of life, we will use a custom or semi-custom ear orthotic to reshape the cartilage of the ear. There's been very good research that has indicated that the cartilage in the ear of a child is moldable for the first six weeks of life, and maybe slightly longer than that in some children. So, we take advantage of this time to correct anomalies which used to require surgical procedures.
We've been able to get some really powerful changes from everything like prominent ear deformity to folded ears to cryptotia [ear cartilage partially buried underneath the side of the head], and a whole series of anomalies that we used to have to say to a parent, "Well, bring the child back to me when they're three years old and I'll do a small surgery."
How does the orthotic work? Is it fastened on for a period of time?
Here’s the interesting thing, if you knew how to correctly just hold the ear in place yourself and you stood there and you held the ear for six weeks, the shape would change, and it would be permanent. But we don't recommend parents to do that in case they are holding it in a way that doesn't look good and then they're upset about it.
In these cases, we like to see the children as soon as possible, but certainly within the first six weeks. And through a system of adhesives, we do fasten an earmold or an ear orthotic to the child's head. The orthotic is then changed out by myself in the office, and this is done on a recurring basis every one to two weeks until the treatment is done. The treatment usually lasts about four to six weeks, and again, the results are permanent.
We’re talking 95-97 percent efficacy with this treatment. In my mind, that's a lot of children who may have been getting surgeries when they're older who are now getting successful non-surgical treatment and doing it at a relatively young age where they'll never have to be cognizant of the fact that this occurred.
Thinking along the lines of seeing the child as early as possible, have there been any developments in prenatal diagnosis?
Oh yes, this is actually a topic I’ve published on. We have a prenatal consult program in conjunction with our colleagues in Maternal Fetal Medicine where we use advanced techniques to help diagnose craniofacial abnormalities in utero. More importantly, that early prenatal consultation for entities like cleft lip and palate, once diagnosed in utero, can actually have a positive effect on the postnatal course for the child and for the mother.
Really, what we're doing is collaborative counseling. The patients will meet with the maternal fetal medicine doctor, a clinical geneticist, and the craniofacial specialists, all at a minimum. We do advanced imaging to help refine the prenatal diagnosis and really give the family as much information about the pregnancy as possible, as early as possible.
But beyond giving information, this collaboration is really fruitful because the data shows that early and appropriate counseling leads to better outcomes once the child is born. We see lower rates of postpartum depression. Better rates of feeding and weight gain in children with cleft lip and palate that had prenatal diagnosis. And certainly, we are able to plug them in earlier with our surgical team to get them prepared for their surgeries.
Incredible. Let’s talk cleft lip and palate. How do you go about developing surgical plans to treat cleft disorders?
This is a topic I’m so very passionate about. So, research shows that children with cleft lip and palate are best taken care of in the context of a multidisciplinary team, and as the term implies, that involves more than plastic surgery.
Here at Columbia, I co-direct our craniofacial team along with one of my colleagues, Dr. Jeffrey Ascherman. But the team really is so much more than us. There are individuals from pretty much every specialty that a child with a cleft lip and palate could need on our team. This includes pediatrics, pediatric ENT. It includes speech therapy, oral surgery, pediatric dentistry, orthodontics, just to name a few.
Does the entire team see the child at the same time, in the same appointments?
Absolutely. It’s so much more efficient. Our kids come to one appointment and all the providers are present. It can certainly be a long day for a little child and a family, but at the end of that day, they have is a multidisciplinary treatment plan from many providers that lays out the important things for the family to do, let's say, over the next six to 12 months before they come back to the team. And that’s all instead of going to multiple appointments over multiple days in different offices.
Is cleft lip and palate generally something that requires a long-term relationship with your team?
It is. You know, generally, cleft lip and palate is an entity where there can be multiple points of care as a child grows up. Our concerns for an infant may be different than our concerns for a toddler and may be different for our concerns for a school-aged child. By the craniofacial team seeing the patient on a recurring basis, we not only set up an escalating treatment plan as necessary, but we also get the opportunity to really grow up with the family and make a lasting relationship that I think is mutually beneficial.
Are there any new developments within the procedure itself? Any new techniques?
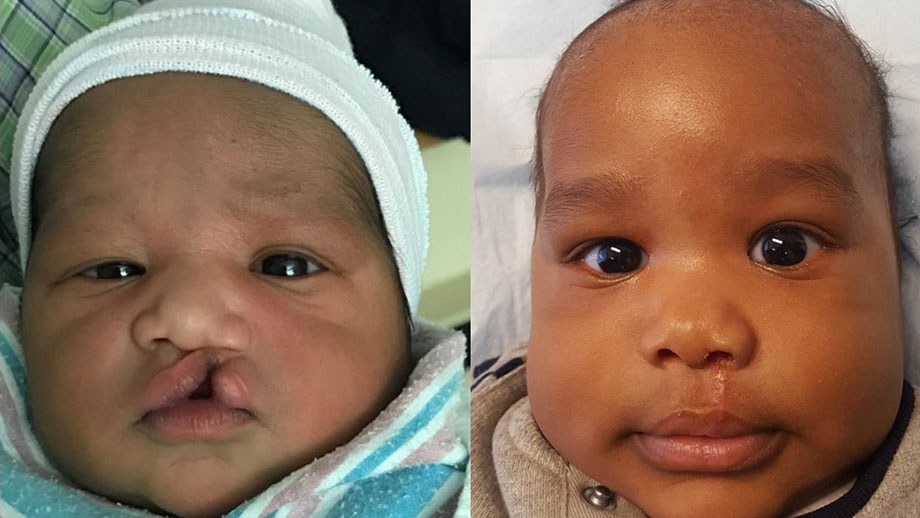
Well first, the two most common procedures that get done are repair of the external cleft lip, which is the upper lip, as well as repair of the palate which is the roof of the mouth. In our offices, these two surgeries will happen during the first year of life, during infancy.
But neonatal cleft lip repair, which is something that I've published on, is a relatively new development in the treatment of cleft lip and palate. We used to think that the treatment of the cleft lip needed to wait until the child was a certain size or a certain age, and oftentimes, children wouldn't reach those criteria until six months or older. Now we take advantage of the fact that we are able to do a lot of prescreening for children, and prenatal diagnosis, that we couldn’t do when we were repairing them many years ago. Through that we're able to find children who are good candidates for neonatal lip repair.
What are the advantages of doing the repair on newborns instead of waiting until they are older?
There really are many advantages. We feel that we get better scarring of the lip repair, and also better contouring of the nasal cartilage during the repair. These are things that are really important for the children and the families long term.
What’s new in the world of research?
There are a lot of new, exciting developments in craniofacial research, both here at Columbia and nationally. But I want to talk about some of the basic science research that's been going on that I'm really excited about. First, in the area of tissue engineering. I spend a lot of time talking about surgery on bone and cartilage and tissues of the facial skeleton. You might imagine that there are some instances where we have a challenge in finding enough bone or tissue to move around and do our procedures. Think, for instance, a patient who comes in after a traumatic accident or a patient who had a bone tumor or malignancy where that bone is now removed. These can be scenarios where it's really challenging to find enough bone elsewhere in the body to replace the bone or soft tissue that was lost.
Certainly, from a surgical perspective, there's been many advanced techniques that have been employed for these procedures over the years, but there's recently been some exciting research going on relating to tissue engineering and 3D printing of craniofacial bioconstructs. Bioconstructs are essentially cartilage scaffolds that can potentially be impregnated with the patient's own live cells, thus making a 3D fabricated replacement for an area of cartilage or bone that has been lost.
Wow, so being able to recreate part of the body with the patient’s own living cells?
Exactly. In some degrees, I think of bioactive constructs as the holy grail in craniofacial research because it really would allow us to refabricate part of the craniofacial skeleton in a way that has such high fidelity with the natural anatomy. It would be such a major advancement. I think some of the basic science research going on here lately has been really forward-thinking, and I'm hoping within the next decade that we will have bioactive 3D printed constructs as a reality.
That’s amazing. What available resources should families know about?
I think the most important thing is that families know what craniofacial specialists do because many times patients don't even realize that we have the skill sets they need to solve their problems. I often see patients who have seen a dermatologist or another doctor, and they don't realize that their problem is a craniofacial problem. Then somehow, they find us. I think patients should know that if they have an issue in the craniofacial area, they should seek out someone who has specific craniofacial expertise because oftentimes we have the appropriate skill set to treat them.
With a lot of the congenital malformations we discussed, are you mostly treating young children or babies because that is the ideal time to treat these disorders? What about older kids who may not have had access to treatment at a younger age?
Great question. You know, the treatment of craniofacial abnormalities, whether they present from a congenital aspect or an acquired aspect, are typically going to be improved by having an assessment as soon as possible. And as soon as possible can range from children to adults. We have patients from age zero all the way through adulthood.
Certainly, I would say that the majority of patients are going to be pediatric, but we see adults that have had trauma. We see adults who need cancer reconstruction after removal of tumors or cancer procedures. We see patients who have developed facial abnormalities secondary to just aging and time. So, in all cases, I think the key is realizing that your issue is in the craniofacial area and then seeking out a craniofacial provider.
That’s one of the great things about being at Columbia, we have great expertise across all disciplines and a really collaborative working environment. With our multidisciplinary team, all of those individuals are able to be accessed through our craniofacial team. Or if you don't need the entire team, the craniofacial plastic surgeon and the other provider can work together independently. We really customize your care.
What excites you most about the future of craniofacial care?
One of the things that has really excited me recently is the recent trend towards trying to change some of the social perceptions around people with craniofacial abnormalities or craniofacial differences. A few recent things happened in the cleft lip and palate advocacy community this past year alone. Several stories caused national conversations to start around some of the stigmata that's attached to cleft lip and palate.
People need to remember that cleft lip and palate is very common, one out of 700 births. You probably know someone that has had a cleft lip and palate but had surgery so you may not be aware of it. It's a really common thing. In the cleft community and the cleft advocacy community, which I consider myself a part of, we’re pushing a lot of campaigns to try to bring social awareness around the more psychosocial challenges that children and families with cleft lip and palate go through.
Here at Columbia, July is always exciting because it’s Cleft Lip and Palate Awareness Month, and we host our annual Cleft Lip and Palate Team Day with patients and their families. It’s really just a day of fun with a loving community that supports each other. This year it will be virtual, but it will still be great.
What are your goals for the next five to 10 years?
From a programmatic standpoint at Columbia, we're really in the midst of growing our team. We have one of the busiest teams in the local region, but we still feel like there is more that we have to offer the patients in the tri-state area and beyond. We have recently hired a craniofacial nurse practitioner who will work in a collaborative manner with our pediatric neurosurgery colleagues at Weill Cornell in a bi-campus role. We’re also expanding research, adding a full-time clinical research coordinator to really get our advances out there to the larger scientific community.
That’s great to hear.
You know, on a personal level, one of my goals is to really highlight some of the incredible journeys our patients have gone through. We have children and their families who have really overcome so much. I'm really proud of them. And I think their stories may serve as motivation for someone else going through or trying to overcome something similar. I think that's the really important work that we're just beginning to facilitate, and I hope to see more of that over the next five years. Our patients are incredible.